Are we getting close to being able to regrow a torn ACL?
We speak to a top surgeon who is exploring a new technique to help some ACL patients heal better and faster
All the latest inspiration, tips and guides to help you plan your next Advnture!
You are now subscribed
Your newsletter sign-up was successful
If you’re a skier (or basketball player, or avid trampoliner for that matter), you probably know that it’s not a matter of if you blow out your knee, but when. For me it was the winter of 2017, my eighth season living in Vail. I was foolishly gliding through early season powder, my ski caught on a hidden log under the snow and didn’t release. You know, the usual story.
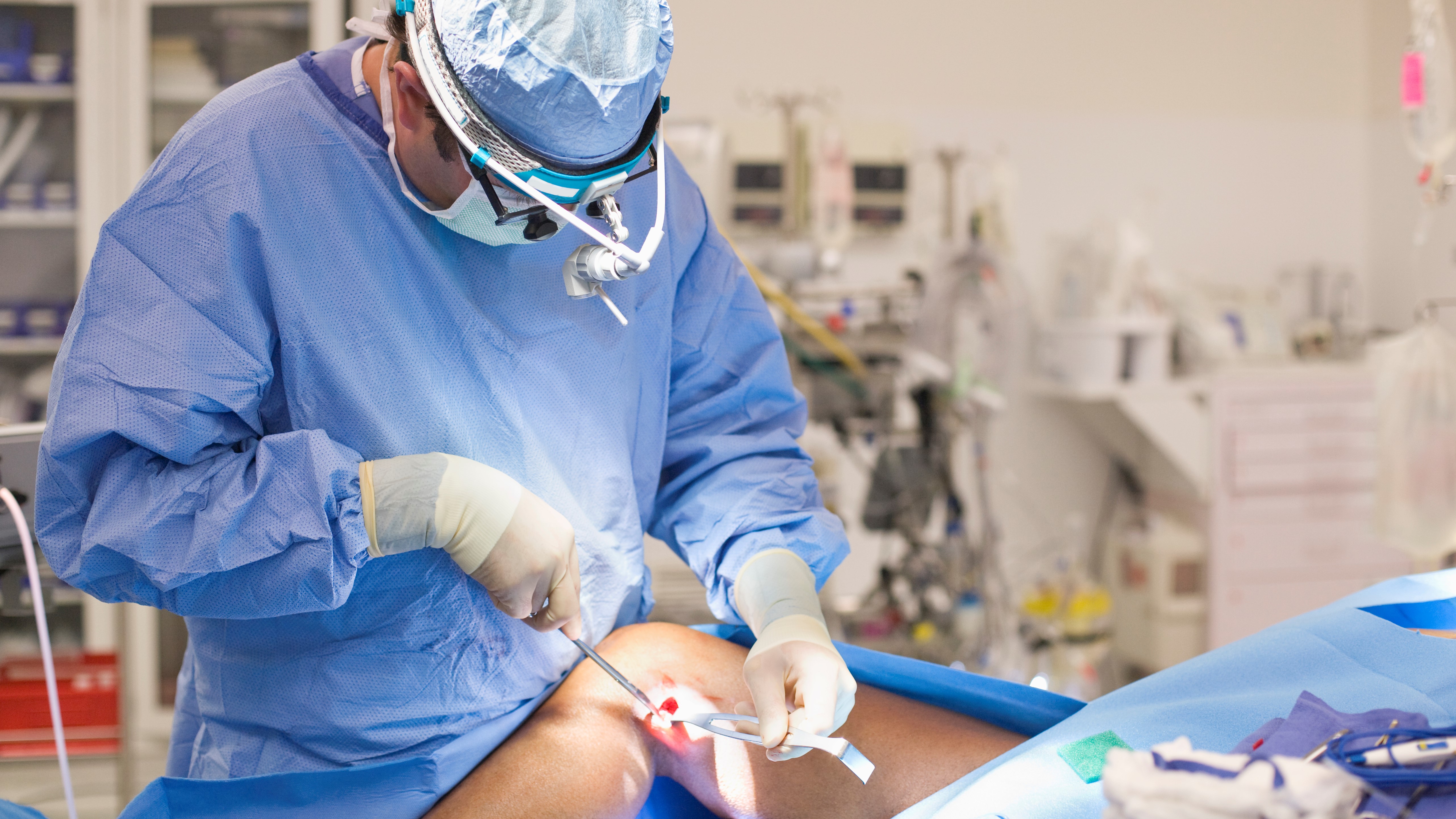
I had my left ACL replaced a couple of months later using a graft from the hamstring tendon on the same leg. It’s a surgery that’s performed some 200,000 times each year in the United States, so I went in thinking I’d just follow the protocols and be back to ship shape in six to nine months, but as I learned when I tore my ACL, just because a surgery is routine, doesn’t mean it’s an easy recovery.
To keep the story short, my 'recovery' entailed two years of pain and only about 80% extension in my knee before I finally had a second procedure to remove loads of scar tissue, hardware, and bone fragments. Within nine months of that surgery, I was finally back in my hiking boots.
My story is surprisingly common, and honestly, many others go through far worse. Today, the very surgeon who cleaned up my knee and got me back on the trail (and even putting in a lot of miles in my trail running shoes these days) is one doctor who is exploring a ground-breaking new method of repairing ACLs that aims to save your ligament. I recently spoke to Dr Richard Cunningham of Vail-Summit Orthopaedics & Neurosurgery about the work he's doing to try to support his patients' natural healing process and how a new technique may significantly reduce recovery time for some patients.
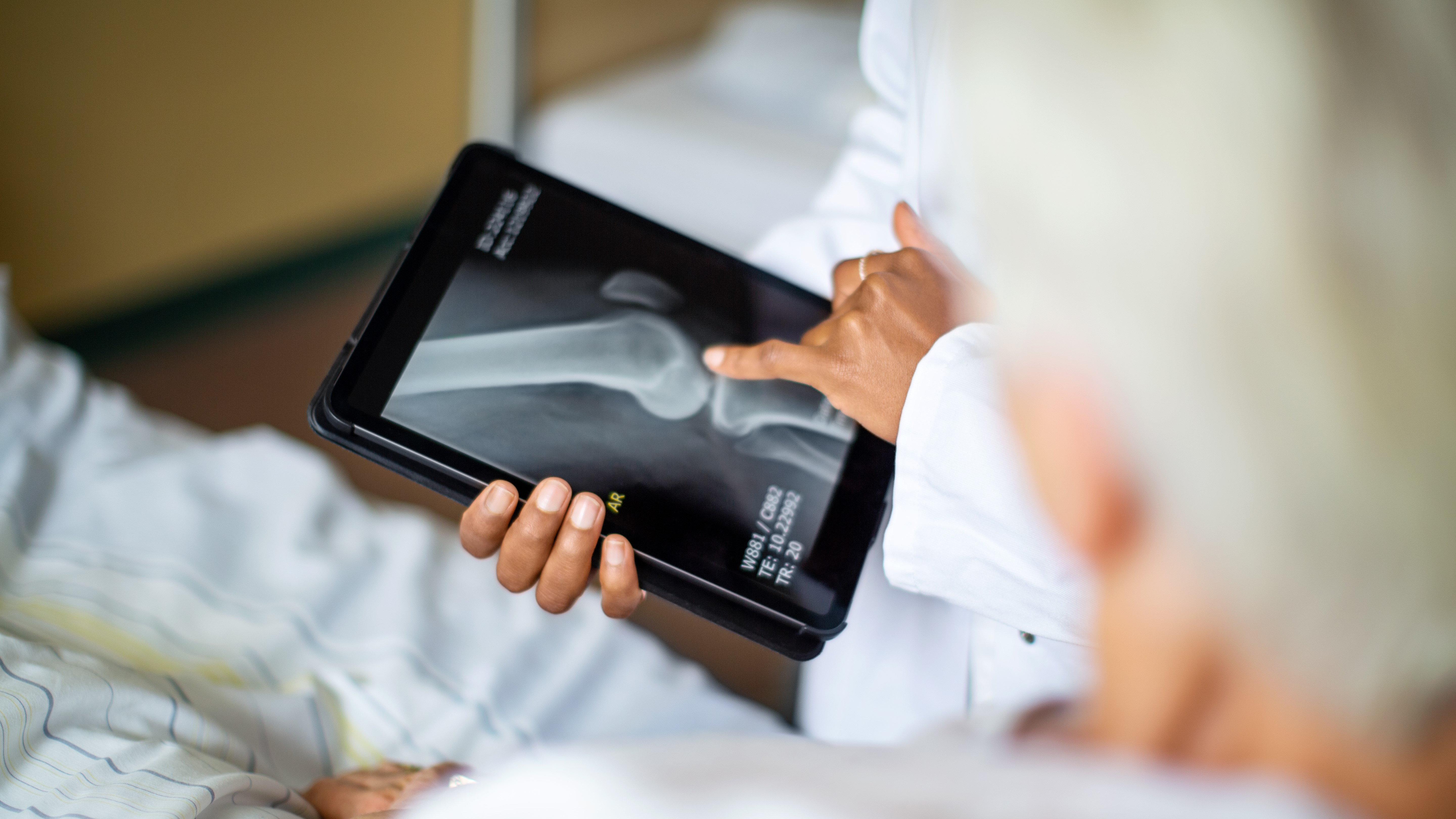
What does traditional ACL replacement entail?
Your ACL (anterior cruciate ligament) is a ligament that helps stabilize your knee, and connects your thigh bone to your shin bone. When you rupture it, it might tear somewhere in the middle, or it may stay intact, but detach from either of those bones. Until recently, an ACL surgery really meant a replacement, involving harvesting tissue from your own hamstring, quad or patella (or taking it from a cadaver), formulating a shiny new ACL and drilling the fraft into your femur and shin. This is problematic because it means that you essentially have two surgeries on the same joint, and in my case I was trying to rehab a knee with a significantly weakened hamstring. In recent years, however, Cunningham has found that he’s been able to save the native ACL in certain cases.
“In tears where the ACL pulls off the femur instead of being torn right in the middle, I've been able to secure it to the bone and get it to heal quite well, much like a rotator cuff repair and the results have been really encouraging,” says Cunningham, a US Ski Team physician who worked with the Pittsburgh Steelers and the Pittsburgh Penguins before joining VSON back in 2003.
“The nice thing with those repairs is that recovery is quicker, it's less invasive, we’re not harvesting a tendon and having to drill sockets in the bone and all that.”
All the latest inspiration, tips and guides to help you plan your next Advnture!
Until recently, this technique has only been applied to ruptures that are higher up on the ACL (known as “proximal tears”), while the so-called mid-substance ruptures, where the ligament is torn in two, have been replaced.
“In the old days we would try to sew those together, but biology wasn't such that the ligament could heal itself well because our joint is a fluid-filled environment. So it would just wash away any kind of healing cells that might migrate to the zone of injury to try to get a ligament to heal.” says Cunningham.
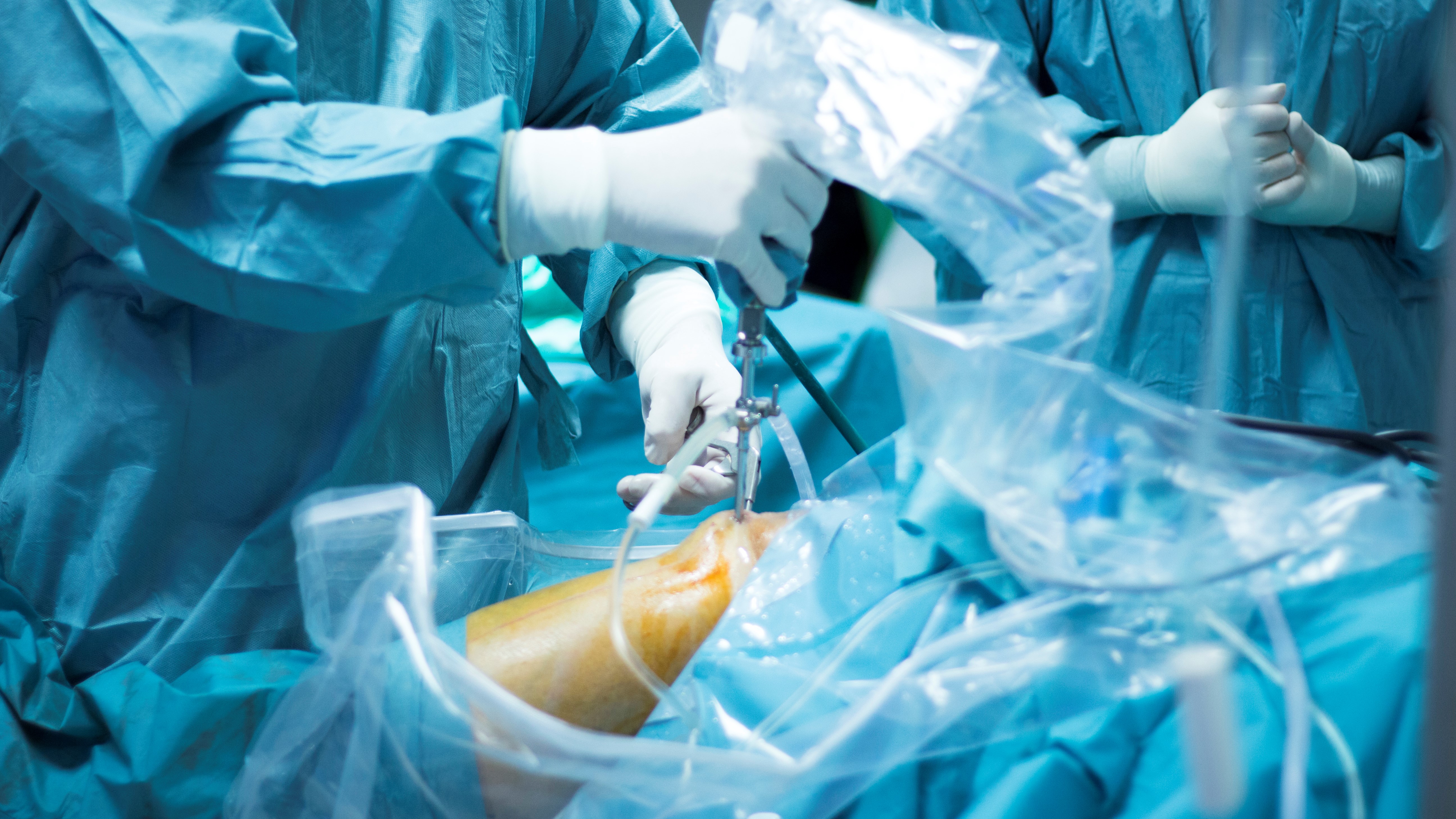
An innovative alternative to traditional ACL surgery
Those types of tears, however, are more common, and figuring out how to apply the repair technique to these cases could be life-changing for many patients. That is where Cunningham, who says he performs up to 120 ACL surgeries a year, is now focusing his efforts. In his Vail practice, he’s been experimenting with Bridge-Enhanced ACL Restoration (the BEAR technique), which was pioneered by pediatric surgeon Dr Martha Murray of Harvard Medical School and Boston Children’s Hospital. According to Duke Health, the BEAR technique, which was approved by the FDA in 2020, uses a bovine collagen implant injected with the patient’s own blood and placed into the gap in the ACL which is then absorbed into the body over eight weeks. Your tendon and surrounding tissue experiences no major disruption to nerve and blood supply and your body gets to harness its own natural healing capabilities. At least, that’s the idea.
Cunningham and his team placed such an implant in a patient with a torn ACL early in 2023 and are now awaiting the long term results to see if the technique could be a valid substitute for a graft. He is quick to stress that this technique is still very much in the experimental stages and he’s taking a conservative approach to it in regard to his own patients, but when we spoke in mid-April, he reported that so far, his test patient was doing well.
“For tears that are within the middle of the ligament, I don't think we're there quite yet, but there is some encouraging data coming out regarding the BEAR. In my own practice I think it's just more of an extension of these ACL repairs that I've been doing, where we secure to the bone, but now we're trying to see if we can cheat that down a little bit and for tears that are farther down.”
Currently, Cunningham is awaiting the results of a new study on the BEAR before he starts to push the envelope for mid-substance ruptures, pointing out that Murray’s work has been with children which may not fully translate to adults.
“I say kids are kind of like salamanders, you know, they heal anything so I'm a little worried that in an adult, are we going to see those same healing rates or are we going to see high failure rates?”

Are there any risks involved with the BEAR technique?
Like any surgical procedure, there are risks involved with the BEAR technique and for Cunningham, an area of concern is that the implant is quite large – three or four centimeters by a centimeter and a half in a part of the body where there isn’t much room to begin with.
“My concern is that it maybe you get a scarring and adhesions and what's called a cyclops lesion where you basically get a big scar ball right in the notch and it impinges and causes pain and you have to go back in and remove it later on down the road,” says Cunningham, who’s been trying to get permission to trim the implant to a smaller size (as the former owner of a cyclops lesion myself, I can attest that it’s not something you want if you can avoid it).

What are the potential benefits of the BEAR technique?
Despite his cautious approach, Cunningham is hopeful that a few years down the line, the BEAR technique will be taking the place of some ACL replacements.
“I think all of it is really great for patients who are young and active because there's the potential that we can save one’s anatomy and not be as invasive and get them back to their activities even faster.”
If the BEAR technique proves to be a suitable replacement for some ACL replacements in adults, it could reduce recovery time by as much as half which means less time off work, less money spent on expensive out-of-network physical therapy appointments, and more time getting back out on the hill and doing what you love most.
Julia Clarke is a staff writer for Advnture.com and the author of the book Restorative Yoga for Beginners. She loves to explore mountains on foot, bike, skis and belay and then recover on the the yoga mat. Julia graduated with a degree in journalism in 2004 and spent eight years working as a radio presenter in Kansas City, Vermont, Boston and New York City before discovering the joys of the Rocky Mountains. She then detoured west to Colorado and enjoyed 11 years teaching yoga in Vail before returning to her hometown of Glasgow, Scotland in 2020 to focus on family and writing.

